Deductibles, copays and coinsurance – oh my!
Let’s be honest. The lingo around health insurance is confusing to most people. But, it’s important to understand some key terms so you can choose the medical plan that works best for you and make the most of your coverage during the year.
Spend a few minutes reading this article. Before you dig in, know which health plan you signed up for (HSA Advantage Plan or Signature Plan). You may want to open a second tab and keep the summary of medical plans open so you can refer back to it as you learn about these terms.
The basics
When you are enrolled in one of our medical plans, you and the health system share the cost for your healthcare expenses. The health system has engaged Blue Cross and Blue Shield to administer our health plans. Prescription coverage is provided as part of both plans with Navitus Health Solutions as the administrator.
Deductibles, coinsurance and copays are examples of what you pay for your share of costs.
What is a deductible?
A deductible is the amount you pay for the cost of healthcare services and prescriptions before the health system begins to pay its share. Your deductible amount varies based on three factors:
- which plan you choose (HSA Advantage Plan or Signature Plan)
- whether you choose coverage for only yourself or yourself and family
- and the network (health system, in-network or out-of-network)
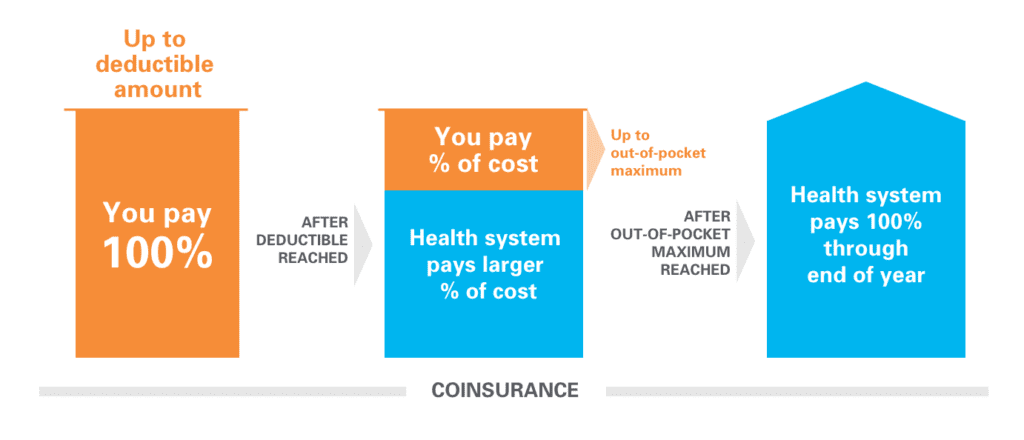
How it works: If your deductible is $1,500, you’ll pay 100% of eligible healthcare expenses until what you’ve paid adds up to $1,500. After that, you “met your deductible” and you share the cost with the health system by paying coinsurance for covered services and prescriptions.
You can read more about deductibles below.
What is coinsurance?
Coinsurance is your share of the cost of a covered healthcare service or prescription after you’ve met your deductible. It’s usually figured as a percentage of the amount allowed to be charged for services.
How it works: You’ve paid $1,500 in healthcare expenses and met your deductible. Now when you go to the doctor, instead of paying the full cost, you and the health system share the cost. For example, if you go to a health system emergency room after you’ve met your deductible, the health system pays 90%. The 10% you pay is your coinsurance.
What is a copay?
A copay is a fixed amount you pay for a covered healthcare service or prescription, usually when you receive the service. The copay amount is different depending on the type of service/prescription and which provider network/pharmacy you use. Copays do not count toward your deductible – you always pay that amount whether you have met your deductible or not until you reach your out-of-pocket maximum (more on that below).
How it works: You see a health system specialist several times a year. At each visit, you will pay a $40 copay even if you have met your annual deductible until your out-of-pocket maximum is reached.
How each plan works
The HSA Advantage Plan uses coinsurance for all covered services and prescriptions. There are no copays with this plan.
The Signature Plan uses copays for in-network office visits and prescriptions, and uses coinsurance for some services after your deductible is met. Note: Copays do not count toward your deductible.
What is the out-of-pocket maximum?
This is the most you’ll ever have to pay for covered services in the calendar year. After you’ve paid this amount, you’ll have no copays or coinsurance – the health system will pay 100% of the cost of all covered services and prescriptions for the rest of the calendar year.
Important fact about preventive care
The health system wants all employees and their families to get the right healthcare services to be well – even if you are already healthy. That’s why the health system pays 100% for preventive care in both plans when you use health system or in-network providers. That means no deductible to meet and no copay or coinsurance for preventive services. So, don’t delay – keep up with your annual physicals and preventive screening exams.
The network your provider is in affects how much you pay for office visits and prescriptions. Your provider will be in one of these networks: · In-network · Out-of-network
|
Resources
Medical coverage:
- Your Blue Cross ID card lists your deductible and out-of-pocket maximum.
- Log in to your health plan account with Blue Cross and Blue Shield (BCBS) or register at MyHealthToolkitKC.com, where you’ll find more tools to understand your medical benefits, find in-network providers and more.
- Use the Blue Cross mobile app to see your plan’s copay/coinsurance amounts. Download My Health Toolkit® for BCBS from your app store.
- Pharmacy coverage:
- Log in or create an account at Navitus.com or in the Navitus mobile app. You’ll have access to a digital ID card, your medication history and more.
- Read more about how to make the most of your pharmacy benefits in several articles in Use Your Benefits.
All benefits:
- Bookmark and continue to visit the Benefits Connection website at https://kansashealthsystembenefits.com/ for benefits information and tips for making the most of your benefits year-round. No password or network access is needed.
More about deductibles
- The phrase “meet your deductible” means paying that amount before the health system begins to pay. After you meet your deductible, your share of cost is coinsurance.
- Your deductible resets to zero on Jan. 1 each year.
- The Signature Plan has an embedded deductible.
- Once any covered member in your family meets their individual deductible, the health system begins to pay its share for that person’s covered services, even if the family deductible has not been met.
- Example: John has employee + spouse coverage and uses health system providers. They each have an annual deductible of $400.
- John has met his deductible of $400. The health system will now pay a portion of his medical expenses for the rest of this year.
- John’s wife Laurie hasn’t had any medical expenses yet this year but went to the emergency room this week. She’ll need to pay the first $400 of the cost since her individual deductible had not been met. Going forward, the health system will pay a portion of qualified expenses for the rest of the year.
- John and Laurie will continue to pay copays for health system and in-network office visits and prescriptions until their out-of-pocket maximum is met.
- The HSA Advantage Plan has an aggregate deductible.
- The full amount of the family deductible must be met before the health system begins to pay for anyone’s services.
- Example: Steve has employee + spouse coverage and uses health system providers. The family deductible is $3,000.
- In January, Steve went to urgent care, filled prescriptions and had several follow-up doctor’s appointments. His medical bills so far total $1,250.
- Steve’s wife Sarah injured her ankle and had several physical therapy sessions, filled prescriptions and visited her specialist. Her medical bills so far total $2,300.
- Together, Steve and Sarah have met their family deductible and the health system will pay a portion of their qualified expenses for the rest of this year until their out-of-pocket maximum is met.
- Steve and Sarah used the $1,000 in seed money the health system put in their HSA to pay part of their cost.
Get support
The Benefits team is here to help you make the most of your benefits. Please call 888-494-9119 with any questions. The phone line is open Monday-Friday, 8 a.m.-5 p.m. CT and there is a Spanish option available. You may also email BenefitsConnection@kumc.edu.
