The medication formulary from Optum Rx (the provider of pharmacy services contracted by Blue Cross and Blue Shield) is different from your current plan which may impact your cost for some prescription medications in 2021.
What you need to do
Understand how the medications you take are covered according to the new formulary. The full formulary for 2021 is not yet available from Blue Cross and Blue Shield. You can review the 2020 formulary here [Formulary – 2020 pdf. ]. We will post the 2021 document as soon as we receive it.
In the meantime, these summary documents for 2021 changes will provide insight to enable an informed decision.
- Formulary Exclusions – 2021 [Formulary Exclusions- 2021 pdf. ].
a. Look for your medications to see if any will be excluded from coverage in 2021.
b. If a medication you take will be excluded, contact your prescriber to develop a plan to switch to a medication that is covered.
c. For Kansas City employees only: if you are currently enrolled in one of the health system’s medical plans, and you currently take a medication highlighted in yellow in the column “Excluded Medications,” the medication will continue to be covered and there is no need to make a change. (Employees in Greater Kansas may disregard the yellow highlights.)
2. If you are considering the Signature Plan, review the document named Formulary Changes – 2021 [Formulary Changes- 2021 pdf.]. This document illustrates medications that are moving into a different tier which will impact current members’ copay for the drug and provides a preview for prospective plan members.
a. Look for your medications to determine what tier they will be in next year.
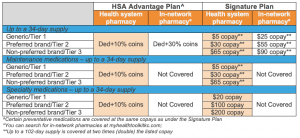
b. Understand the copay amount by reviewing the chart at the bottom of this email.
c. If your medication is in a higher tier, consider whether you want to work with your prescriber to switch to a preferred alternative medication (listed in Formulary Exclusions – 2021 in the column labeled “Preferred Alternatives”).
Timeline
You have until January 1, 2021, to make medication changes related to the new formulary. Until then, your current medical plan coverage applies.
Maintenance and Specialty Medications
We want to take this opportunity to remind you of key changes beginning January 1 for:
• Maintenance medications – long-term, regular use to treat chronic health conditions. In 2021, you must have these medications filled by one of the pharmacies listed below to receive coverage. Any amount you pay outside of these pharmacies will not apply toward your deductible or out-of-pocket maximum.
– The health system pharmacy
For employees in Greater Kansas only:
– Reed Pharmacy in Larned and Sterling
– The Medicine Shoppe in Great Bend
• Specialty medications – high-cost drugs to treat chronic or complex health conditions. In 2021, the health system pharmacy will be the exclusive provider for specialty medications for employees at all locations. You will be required to fill prescriptions for specialty medications via the health system pharmacy.
The health system pharmacy offers online fills and transfers as well as home delivery. You will receive communication in November about how to transfer prescriptions by January 1.
Summary of employee cost for prescriptions in both medical plans (click here [ Interactive Benefits Guide ] for the full benefits guide)